Pelvic Floor Therapy for Gut Health!
- Nov 11, 2021
- 10 min read
Click HERE to watch a video version of this blog where Dahlia Marin, RDN, LD, and Dr. Kat Wong, DPT discuss pelvic floor and the gut!
The pelvic floor refers to the muscles at the bottom of the pelvis, spanning from the pubic bone to the coccyx. These muscles act like a hammock, supporting the bowel, bladder, and reproductive organs. The pelvic floor serves five (5) main functions:

Supporting the organs that rest in your abdomen and help your pelvis against gravity and added downward pressure
Stabilize your “core” muscles. The pelvic floor muscles work in opposition to your diaphragm and provide an environment for efficient automatic core engagement
The sphincter muscle of the pelvic floor contracts when there is an increase in abdominal pressure (which occurs when you cough, sneeze or jump) to help prevent leakage from the bowel. This same muscle relaxes when you urinate or have bowel movements.
Facilitate sexual performance: the pelvic floor is crucial to achieve and sustain an erection and is necessary for orgasm.
The pelvic floor acts as a Sump Pump: it helps pump blood from the pelvis to decrease swelling or pelvic congestion.
Gut health can greatly affect the pelvic floor and vice versa. Unbalanced gut health can lead to symptoms such as constipation and diarrhea. The muscles of the pelvic floor can become weakened (hypotonic) or extremely tight (hypertonic). A weak pelvic floor may lead to incontinence, while a tight pelvic floor can cause constipation and pain. In this blog, we will look at the various factors that affect gut health and the pelvic floor.
Inflammation
Normally, inflammation is the body’s natural damage control. It occurs in reaction to infection, activating white blood cells to initiate a cascade of molecules including histamines. In certain conditions, like autoimmune disorders, the body initiates inflammations against its own cells, causing pain and various other problems throughout the body. Inflammatory pain is hypersensitivity due to tissue damage caused by the inflammatory response. The intensity, duration, and frequency of the pain can become exaggerated if inflammation is left unaddressed.

Lifestyle factors can also influence inflammation in the body. These factors include:
Lack of movement
Environmental exposures including pesticides
Molds
PFEs, PFOAs, PTFEs, and other harmful substances
Chemicals found in cleaning products
Lack of sleep/nervous system rest
Stress
Substance abuse
Excessive screen time
Diet can also influence inflammation in the body. Poor quality diets are associated with increased oxidative stress and altered glucose/lipid metabolism in our adipose tissues, muscles, and liver. Certain foods can increase or decrease inflammation. If your goal is to address chronic inflammation, consume a variety of colorful, fiber-rich foods as well as foods containing omega-3 fatty acids and make sure you stay well hydrated. Your lifestyle habits can also influence inflammation. Make sure you exercise regularly and find activities that help you to de-stress like being in nature or around animals. Get sufficient sleep and be gentle with yourself to allow for optimal healing.
Just as some foods can help reduce inflammation, others can exacerbate it and worsen symptoms. Diets high in refined carbohydrates, alcohol, saturated fats, and animal proteins can increase inflammation and influence discomfort or pain. If you are experiencing inflammation, it may be due to the quality of your diet and lifestyle. The foods you consume may be reacting negatively with your immune system, and certain compounds in your food may be exacerbating inflammation:
Histamine is a chemical that is released by your mast cells when they encounter allergens. If you are frequently consuming foods that increase histamine production including fermented beverages and foods, dried fruits, avocado, eggplant, spinach, processed meats, and many others. In the body, Diamine oxidase (DAO) is an enzyme responsible for breaking down histamine. Some individuals may be deficient in DAO due to medications that block its function or prevent its production, GI disorders including leaky gut and IBD, or foods that impair or block DAO from functioning properly.
Oxalate or oxalic acid is a naturally occurring compound found in many plant foods. When consumed in moderation, oxalate-rich foods are beneficial for your health. These foods include peanuts, spinach, beets, sweet potatoes, rhubarb, and even chocolate! However, excess oxalates have the tendency to combine with calcium in your urine and can cause kidney stones or kidney damage. High oxalate foods can trigger inflammation and pain, irritating tissues and mucous membranes.
Salicylates are naturally occurring in many fruits and vegetables. They act as a preservative, to prevent rotting and protect against bacteria and fungi. They are stored in the leaves, seeds, bark, and roots of plants. Salicylates are found naturally in many foods and are used in products as preservatives. Excess salicylates can cause stomach pain, blood in vomit, stools, or urine, bruising or bleeding, swelling, and rashes/itchy skin.
Lectins are proteins (also called hemagglutinins) that bind to carbohydrates. They occur naturally in plants, but plant foods like peas, lentils, beans, soy, and peanuts contain the highest amounts. These proteins can cause issues when we try to digest them because they are more resistant to the acidic environment of our stomach. The acid-resistant property of lectins help protect plants from pests, but can also cause digestive issues for us when we try to consume these lectin-rich foods. Lectins can cause GI issues in some individuals, especially when these foods are undercooked. Gas, bloating, nausea, vomiting, and diarrhea are all side effects of consuming foods high in lectins.
Gluten refers to proteins found in many types of wheat, barley, spelt, and rye. The two main proteins in gluten are gliadin and glutenin. Gliadin is the protein that causes adverse reactions in those with celiac disease or gluten sensitivity. Gluten is found in a wide variety of foods, including some you would not expect. Foods containing gluten include bread, pasta, cakes and pastries, crackers, vegetarian meat substitutes, malt extracts and syrups, gravies and sauces, soy sauce, processed meats, chips, cereals, beers, and more.
Bloating and Distention
Bloating is the sensation of abdominal swelling that is a common and ultimately normal process. Bloating is a cumulative process that occurs in response to your diet and lifestyle practices throughout the day. High fiber diets can cause bloating, but excessive gas (passing gas more than 15-20 times a day), malodorous gas, and abdominal pain are worrisome signs to take note of. While it is normal to experience uncomfortable bloating during your menstrual cycle (due to progesterone and estrogen fluctuations), it is not normal for painful bloating to occur frequently. Waking with bloat or constipation can be signs of histamine intolerance, dysmotility (malfunction of the movement of your digestive tract) or dysbiosis (a reduction in gut microbiome diversity) could be causing more serious issues in your gut. Distension, as opposed to bloating, is the measurable increase in abdominal size. Abdominal distension can be caused by constipation, conditions like IBS, or having an enlarged bladder. Click HERE for information on carminative herbs that can help alleviate bloating and gas.
Constipation
Constipation occurs when stool is moving too slowly through the GI tract, causing the stool to become hard and dry. Constipation can be uncomfortable or even painful and can be caused by certain medications, lack of fluids in the diet, lack of fiber in the diet, conditions like IBS and other issues with GI functions, hypertonic pelvic floor muscles, and stress. Pelvic floor physical therapy can help with chronic constipation by helping to retrain those muscles to relax to allow stools to pass more easily.

Irritable Bowel Syndrome (IBS)
Please see our 3-part series for all things IBS:
Interstitial Cystitis (IC)
Interstitial cystitis is a chronic condition that causes bladder pain and pressure. It can also cause pelvic pain in some individuals. Pain experienced by those with IC can range from mild to severe. IC condition is one of a spectrum of diseases that is known as painful bladder syndrome. Interstitial cystitis signs and symptoms include:
Pelvic pain: In women, pain can occur between the anus and the vagina. In men, pain occurs between the anus and the scrotum. This pain can be chronic.
Persistent or urgent need to urinate, as well as frequent urination throughout the day sometimes upwards of 60 times in one day
Discomfort or pain when the bladder is filling and relief upon urination
Painful intercourse

Signs and symptoms of IC can resemble that of chronic urinary tract infections, however, no infection is present (typically). That said, symptoms of IC worsen if there is a urinary tract infection present.
Risk factors of IC include:
Gender: Women are diagnosed with interstitial cystitis more often than men. In men, symptoms may be similar to interstitial cystitis but are more associated with prostatitis (inflammation of the prostate gland).
Age: A majority of individuals with interstitial cystitis are diagnosed in their thirties (or older).
Preexisting chronic pain disorders: Interstitial cystitis is often associated with other chronic pain disorders, including fibromyalgia, IBS, prostatitis, or vulvodynia.
Most individuals experiencing IC also struggle with sensitivities to certain foods. Many individuals who have IC that also have other health conditions will have to limit or avoid specific foods related to these other health problems. Foods or beverages that trigger IC symptoms are different for everybody.
Foods that are more likely to trigger IC flares:
Acidic beverages, including coffee and tea (caffeinated and decaffeinated), soda, alcohol, cranberry juice, and citrus fruit juices.
Artificial sweeteners
Spicy foods
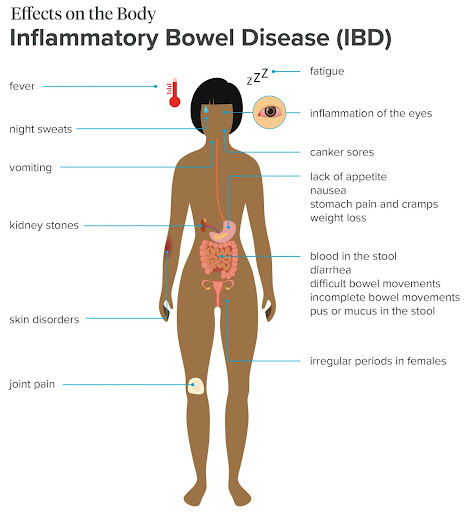
Inflammatory Bowel Disease (IBD)
Please see our blog on World IBD Day: Crohn’s and Colitis HERE
Dietary Tips for Addressing These Conditions
These conditions present many difficulties and frustrations for those who suffer from them. Since these conditions all relate to the digestive tract, urination, and defecation, living with them can feel extremely isolating. Many with these conditions may instinctively restrict any foods that they feel create more symptoms, thus limiting their diets greatly. Healing the gut and creating an environment where different foods are tolerated, is better than prolonged restrictions of various foods. It is important to have a wide variety of foods to get as many nutrients as possible. Addressing the root cause of these conditions can help you to begin tolerating and enjoying more foods and help nourish your body. If you are struggling with these conditions, start with low fiber food and slowly reintroduce each food to increase your tolerance through cooking, freezing, or blending to break down fiber. Get in contact with a knowledgeable professional for guidance on how to improve your gut health!
Sexual Health, Diet, and the Pelvic Floor
Prostate Inflammation or enlargement of the prostate can occur for a variety of reasons, including bladder dysfunction or outlet obstruction, aging, infection or trauma, diet and lifestyle factors including smoking, high fat and animal proteins in the diet, and limited physical activity. The incidence of prostate inflammation is significantly higher in men with metabolic syndrome. Metabolic syndrome consists of symptoms like increased blood pressure, high blood sugar, excess body fat around the waist, and abnormal cholesterol or triglyceride levels.
Disease of the prostate is known as prostatitis. Prostatitis is a disease of the prostate that results in pain in the groin, painful urination, difficulty urinating and other symptoms. Bacterial infections or nerve damage caused by trauma like surgery or injury to the groin area can cause prostatitis leading to inflammation. Acute bacterial prostatitis can be caused by some common strains of bacteria including E. coli, P. Aeruginosa, and Klebsiella species. Infections start when bacteria from urine leak into the prostate.
Pelvic floor hypertonicity can be caused by prostatitis, due to factors including prolonged incontinence which can lead to frequent tightening of the pelvic floor muscles in an effort to prevent urine leaking out. This can lead to pain and increased inflammation of the prostate
Erectile Dysfunction (ED)
Erectile dysfunction is described as difficulty to achieve or maintain an erection firm enough for intercourse. This condition can arise due to a variety of health and lifestyle factors, including:
Heart disease and atherosclerosis
Metabolic syndrome — a condition involving increased blood pressure, high insulin levels, central adiposity, and high cholesterol
Diabetes
Obesity
Certain prescription medications including:
Diuretics
Antihypertensives
Antihistamines
Antidepressants
Muscle relaxants
Tobacco/Alcohol/Substance abuse
Erectile dysfunction is often considered to be an indicator of an individual's risk of developing cardiovascular disease, this is because penile arteries are smaller in diameter than coronary arteries, approximately 1-2 and 3-4 mm in diameter, respectively. Therefore, they are affected by conditions like atherosclerosis earlier than blood vessels in other areas of the body. Studies show that having a HgA1c >5.7% and fasting blood glucose >110 mg/dL is associated with a significant risk for the development of erectile dysfunction. Hyperlipidemia, characterized by cholesterol levels >200 mg/dL, triglycerides >150 mg/dL, LDL >130 mg/dL, and HDL <40 mg/dL, can also contribute to ED. This condition poses a significant risk for atherosclerotic damage to penile blood vessels, therefore increasing the risk for the development of ED. ED is often thought of as the “canary in the coal mine” in terms of risk for cardiovascular diseases, as it typically develops 2-3 years prior to the onset of angina (chest pain) and 3-5 years prior to the onset of cardiovascular disease. Pelvic floor physical therapy can help alleviate ED by addressing pelvic girdle dysfunction and pudendal nerve mobility.
Next Steps
How to implement this information in your everyday life: Start by including more anti-inflammatory foods and lifestyle interventions appropriate for your symptoms/ situation. Assess where you can reduce inflammatory dietary and lifestyle habits Evaluate if any of this information resonates with you and reach out to a professional if you feel you may benefit from our help!
Click HERE to access more informative blogs from www.Marriedtohealth.com
If you are interested in working with an RDN, we would love to support you! You can schedule a personalized visit with us and we would love to collaborate with you on your journey! We see clients from all over the world. Follow us @MarriedtoHealth and join our newsletter so you never miss a #GoodGut thing!
References
Weinstock, L. B., Klutke, C. G., & Lin, H. C. (2008). Small intestinal bacterial overgrowth in patients with interstitial cystitis and gastrointestinal symptoms. Digestive diseases and sciences, 53(5), 1246–1251. https://doi.org/10.1007/s10620-007-0022-z
Abernethy, M. G., Rosenfeld, A., White, J. R., Mueller, M. G., Lewicky-Gaupp, C., & Kenton, K. (2017). Urinary Microbiome and Cytokine Levels in Women With Interstitial Cystitis. Obstetrics and gynecology, 129(3), 500–506. https://doi.org/10.1097/AOG.0000000000001892
Espinosa-Marrón A, Quiñones-Capistrán CA, Rubio-Blancas A, Milke-García MP, Castillejos-Molina RA. Hyperglycemia: the metabolic syndrome component that aggravates erectile dysfunction in Mexican patients. Rev Mex Urol. 2019;79(6):pp 1-12.
Robert J. Ostfeld, Kathleen E. Allen, Karen Aspry, Eric J. Brandt, Aaron Spitz, Joshua Liberman, Danielle Belardo, James H. O'Keefe, Monica Aggarwal, Michael Miller, Columbus Batiste, Stephen Kopecky, Beth White, Nikhil Shah, Hussam Hawamdeh, Travis Batts, Ron Blankstein, Koushik Reddy, Dean Ornish, Andrew M. Freeman, Vasculogenic Erectile Dysfunction: The Impact of Diet and Lifestyle, The American Journal of Medicine Volume 134, Issue 3, 2021, Pages 310-316, https://doi.org/10.1016/j.amjmed.2020.09.033.
Porter, Corey M.; Shrestha, Eva; Peiffer, Lauren B.; Sfanos, Karen S. (2018). The microbiome in prostate inflammation and prostate cancer. Prostate Cancer and Prostatic Diseases. doi:10.1038/s41391-018-0041-1
Abernethy, M. G., Rosenfeld, A., White, J. R., Mueller, M. G., Lewicky-Gaupp, C., & Kenton, K. (2017). Urinary Microbiome and Cytokine Levels in Women With Interstitial Cystitis. Obstetrics and gynecology, 129(3), 500–506. https://doi.org/10.1097/AOG.0000000000001892
Mayo Clinic Staff. (2021, August 21). Erectile dysfunction. Mayo Clinic. Retrieved November 10, 2021, from https://www.mayoclinic.org/diseases-conditions/erectile-dysfunction/symptoms-causes/syc-20355776?utm_source=Google&utm_medium=abstract&utm_content=Erectile-dysfunction&utm_campaign=Knowledge-panel.
Mayo Clinic Staff. (2020, January 17). Prostatitis. Mayo Clinic. Retrieved November 10, 2021, from https://www.mayoclinic.org/diseases-conditions/prostatitis/symptoms-causes/syc-20355766.
Mayo Clinic Staff. (2020, November 7). Inflammatory bowel disease (IBD). Mayo Clinic. Retrieved November 10, 2021, from https://www.mayoclinic.org/diseases-conditions/inflammatory-bowel-disease/symptoms-causes/syc-20353315.
Walfish, A. E., & Companioni, R. A. C. (2021, November 4). Overview of inflammatory bowel disease - gastrointestinal disorders. Merck Manuals Professional Edition. Retrieved November 10, 2021, from https://www.merckmanuals.com/professional/gastrointestinal-disorders/inflammatory-bowel-disease-ibd/overview-of-inflammatory-bowel-disease.
The Facts About Inflammatory Bowel Diseases. New York, NY: Crohn’s and Colitis Foundation of America; 2014. http://www.crohnscolitisfoundation.org/assets/pdfs/updatedibdfactbook.pdf pdf icon[PDF-2.32MB]external icon.
Ktori, S. (2021, April 13). Diet rich in animal products, processed foods, alcohol and sugar linked with inflammatory gut microbiome. GEN. Retrieved November 10, 2021, from https://www.genengnews.com/news/diet-rich-in-animal-products-processed-foods-alcohol-and-sugar-linked-with-inflammatory-gut-microbiome/.
Shorter, B. (2019, March 22). Interstitial cystitis and Diet. Interstitial Cystitis Association. Retrieved November 10, 2021, from https://www.ichelp.org/living-with-ic/interstitial-cystitis-and-diet/.




Comments